Blog
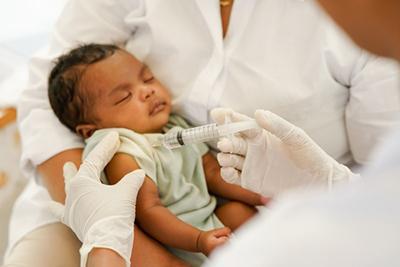
The Importance of Immunizations
- posted: May 01, 2024
Children are surrounded by bacteria and viruses. Some of these bacteria and viruses can cause serious, even life-threatening diseases like meningitis, hepatitis, and tuberculosis. Immunizations safeguard your child’s health, and Read More
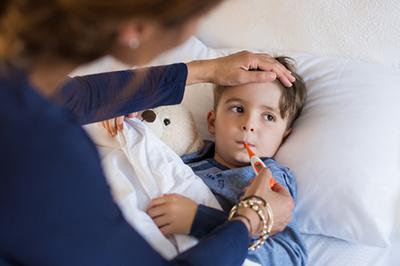
When Should You See Your Pediatrician?
- posted: Apr. 12, 2024
As parents, it's natural to feel concerned about your child's health and well-being, especially when they're experiencing symptoms or discomfort. While many childhood illnesses and injuries can be managed at Read More
How Often Should My Child Be Seeing a Pediatrician?
- posted: Apr. 01, 2024
Here’s the scoop on why you should be bringing your little ones in to see a pediatrician regularly. It's important that you make time to bring your children in to see Read More
What To Expect at a Behavioral Health Evaluation
- posted: Mar. 12, 2024
As a parent, it’s only natural to be curious about your child’s behavior. Is your child’s behavior normal, or is it a sign your child needs help? A behavioral health Read More
The Importance of Regular Well Visits
- posted: Mar. 01, 2024
You want to safeguard your child’s health, but you can't do it alone. You need some help. Regular well visits to your pediatrician can protect your child’s health by providing Read More
The Importance of Early Childhood Vaccinations
- posted: Feb. 07, 2024
Children are one of the most vulnerable age groups because a child’s immune system is not as well developed as that of an adult. Early childhood vaccinations play an important Read More
Childhood Obesity: Causes, Risks, and Strategies for Prevention
- posted: Feb. 01, 2024
Childhood obesity affects approximately 30% of children in the U.S., and numbers continue to rise. According to the Centers for Disease Control and Prevention (CDC), obesity is one's body mass Read More
Best Ways To Prevent Ear Infections
- posted: Jan. 07, 2024
Ear infections are common in children because their ears are not fully developed, and it can be difficult to properly drain fluid. Ear infections can be brutal, and it can Read More
The Role of Pediatricians in Early Childhood Development
- posted: Jan. 01, 2024
Monitoring your child’s development is an important part of what a pediatrician does. It’s important to visit your pediatrician, because child development is a complex area and needs the expertise Read More
Promoting Mental Health in Children
- posted: Dec. 07, 2023
You want your child to be healthy, and an important part of good health is great mental health. Promoting mental health in your child is one of the most important Read More
Tips To Help Your Child Eat Healthier
- posted: Dec. 01, 2023
Caring for your child involves many decisions each day. One of the most important things that you can do is ensure that they’re getting the right nutrition and that they’re Read More
Sports Injuries in Kids: Prevention and Treatment
- posted: Nov. 07, 2023
Child sports injuries refer to physical harm in children while participating in sports and recreational activities. They can range from minor bruises to painful conditions, affecting muscles, bones, and joints. Read More
The Importance of Well Care Visits for Adolescents
- posted: Nov. 01, 2023
Find out why visiting the pediatrician is just as important for teens. We all know just how important it is to bring newborns and children to the pediatrician’s regularly, but we Read More
Asthma Prevention: A Pediatrician's Guide to Respiratory Health
- posted: Oct. 12, 2023
An asthma attack can be scary, especially if it happens to your child. There are some steps you can take to help prevent an asthma attack. Our pediatrician can tell Read More
Why Is A Sports Physical So Important?
- posted: Oct. 01, 2023
When your child wants to participate in their favorite sports, it’s important that you’re doing all that you can to keep them protected. Not only do they need all of Read More
Common Childhood Illnesses
- posted: Sep. 08, 2023
Your child comes into contact with millions of microscopic viruses and bacteria daily. Your child’s immune system also isn’t as robust as that of an adult. These two factors combine Read More
Monday - Friday
9:00 am - 5:00 pm
Saturday
9:00 am - 4:00 pm
one location is open every other Saturday
(call office for details)
Sunday
Closed